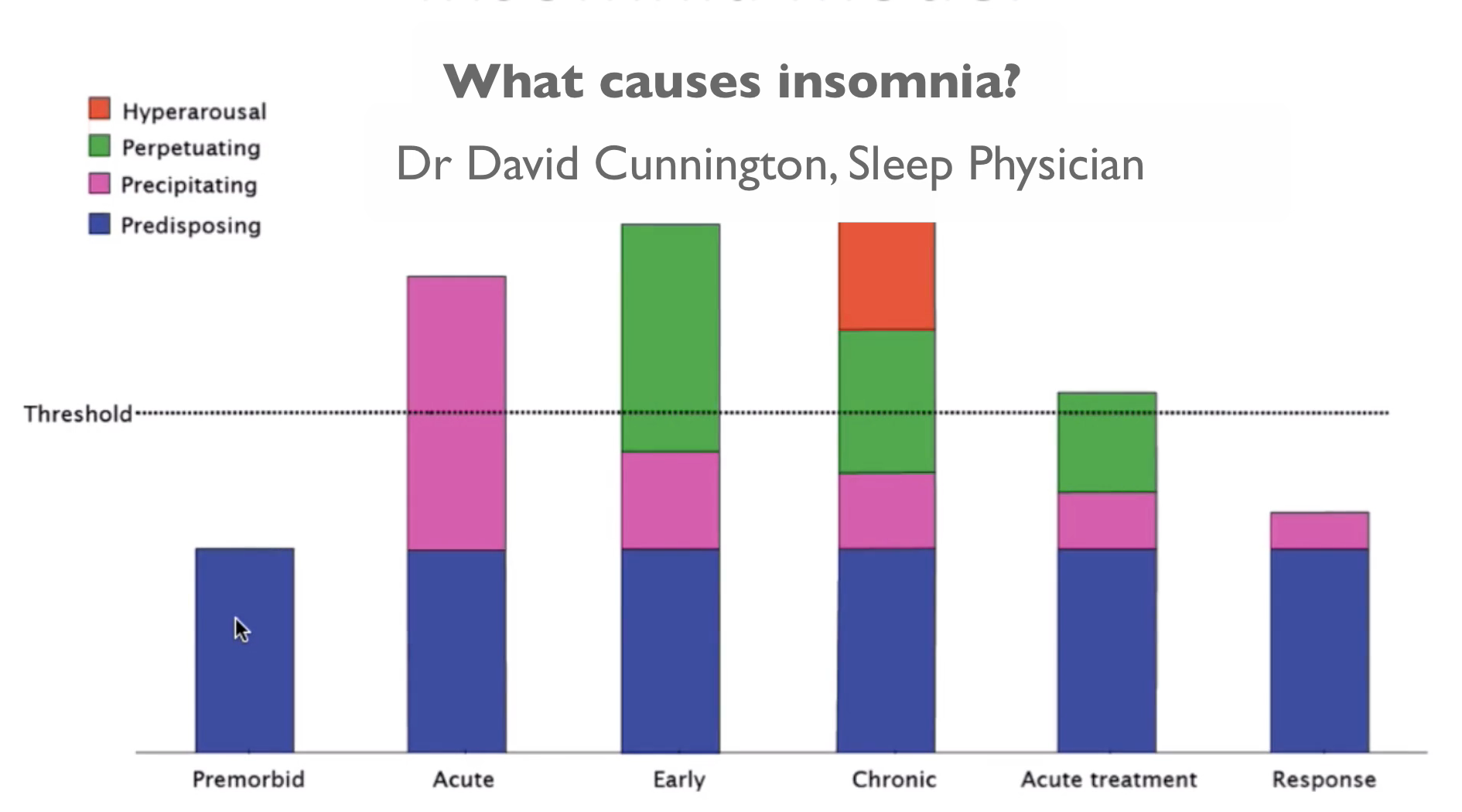
What causes insomnia?
What is insomnia?
Insomnia refers to problems getting to sleep, staying asleep or waking up too early. It can also refer an experience of poor-quality sleep, causing daytime fatigue or sleepiness. In clinical practice, health professionals make the distinction between acute insomnia, which is short term and relatively common (affecting up to 50% of the population), and chronic insomnia which persists for more than three months and causes a significant degree of distress (affecting 10-15% of the population).
For more information on insomnia please see our page What is Insomnia?

What causes insomnia?
It is very important to understand what is causing your insomnia, to ensure you that you get the correct treatment.
There can many different causes of insomnia including: medical conditions, mental health conditions, lifestyle factors, unhealthy sleep habits, and sleep anxiety.
Medical conditions
There are a range of medical conditions that can cause insomnia. Some conditions directly cause insomnia whereas other conditions have symptoms (e.g. pain) that make it difficult to sleep. Medical conditions that can cause insomnia include:
- conditions that cause breathing problems (e.g. Asthma, Chronic Obstructive Pulmonary Disease)
- conditions that cause chronic pain (e.g. arthritis, back pain, migraine)
- acid reflux disorder
- nasal allergies, sinusitis and rhinitis (e.g. hayfever)
- abnormal thyroid function (e.g. hyperthyroidism)
- neurological conditions (e.g. Parkinson's disease)
- other sleep disorders (e.g. Sleep apnoea, restless legs syndrome)


Medications
Certain medications you may be taking for other health complaints can cause sleeplessness. It is important to talk to your GP about the medications you take and how you can manage any side effects they may produce. Some examples of medications that are known to have an effect on sleep include:
- beta blockers for heart conditions
- steroid medication
- allergy medication
- cold and flu tablets or decongestants
Mental health conditions
Insomnia is a symptom of a number of mental health conditions, such as:
- depression
- anxiety disorders
- schizophrenia
- bipolar disorder
- ADHD
If you have experienced any of these conditions it is important to seek the advice of qualified psychologist or other mental health professional to discuss what treatments are available for you.
These conditions can be treated and well managed, and there are many resources available online, through public mental health services and with psychologists or other mental health professionals working in private practice. A list of mental health services are available here.

Important....
Insomnia can be a symptom of another mental health condition, such a depression, but it can also occur as a condition in its own right. In other words, it is common to have a Depressive Disorder and an Insomnia Disorder at the same time.
This means, both the Depression and Insomnia should be addressed in treatment.
Untreated insomnia may increase the risk of relapse of depression, so it's important to talk to your mental health professional about getting specific help for your insomnia as part of your broader mental health treatment.
Lifestyle factors
There are a number of habits, behaviours and lifestyle factors that can contribute to sleep problems. These include
- having a stressful or busy daytime schedule
- inadequate time to wind down before going to bed at night
- drinking too much coffee, tea or energy drinks can interfere with sleep, due to the stimulating effects of caffeine
- eating chocolate at night time (sugar and caffeine)
- drinking too much alcohol
- smoking cigarettes or taking recreational drugs
- having irregular sleep patterns such as going to bed or getting up at different times during the week.
- taking naps of more than 30 minutes during the day
- working late, watching TV or using electronic screens too close to bedtime


Sleep anxiety
Lying awake in bed for hours overnight can be distressing, and many people worry about feeling tired or irritable the next day.
Sometimes just thinking about sleep can make you feel anxious, as you anticipate another night of lying awake all night.
Anxiety about sleep is very common for people who have had insomnia for many weeks, yet unfortunately it has the effect of alerting the body (hyperarousal) and making the problem worse. Sleep anxiety causes increases in neurotransmitters and hormones that keep you awake, making it even harder to get to sleep. Sleep anxiety is part of the vicious cycle of insomnia, and one of the reasons sleep problems can go on for so long.
How does insomnia develop?
These medical, mental health, and lifestyle factors, can cause short term or long term sleep problems. So how does acute insomnia develop beyond a few weeks to become chronic insomnia, lasting several months to many years?
Watch this video to learn how chronic insomnia develops.
Your GP can assess whether there are any underlying medical or mental health issues causing your insomnia, and help you decide on the next steps for treatment. For long-term improvements in sleep talk to your GP about non-drug treatments such as cognitive behavioural therapy and mindfulness training.

What is the best treatment for insomnia?
The most effective long-term treatment for insomnia is cognitive behavioural therapy for insomnia (CBTi) or a newer development of CBTi which includes comprehensive mindfulness training, called Mindfulness-based CBTi, which is the approach taught in our online program A Mindful Way to Health Sleep.
For more information on how to overcome chronic insomnia, please read our page: The best treatments for insomnia.
IMPORTANT NOTE: If you have experienced disturbed sleep for more than 2 weeks and do not know the cause of the insomnia, it is recommended that you see your GP for an assessment and medical check-up. This information is not a substitute for proper assessment and treatment with a suitably qualified health professional.